Elsevier, The Lancet Planetary Health, Volume 5, September 2021
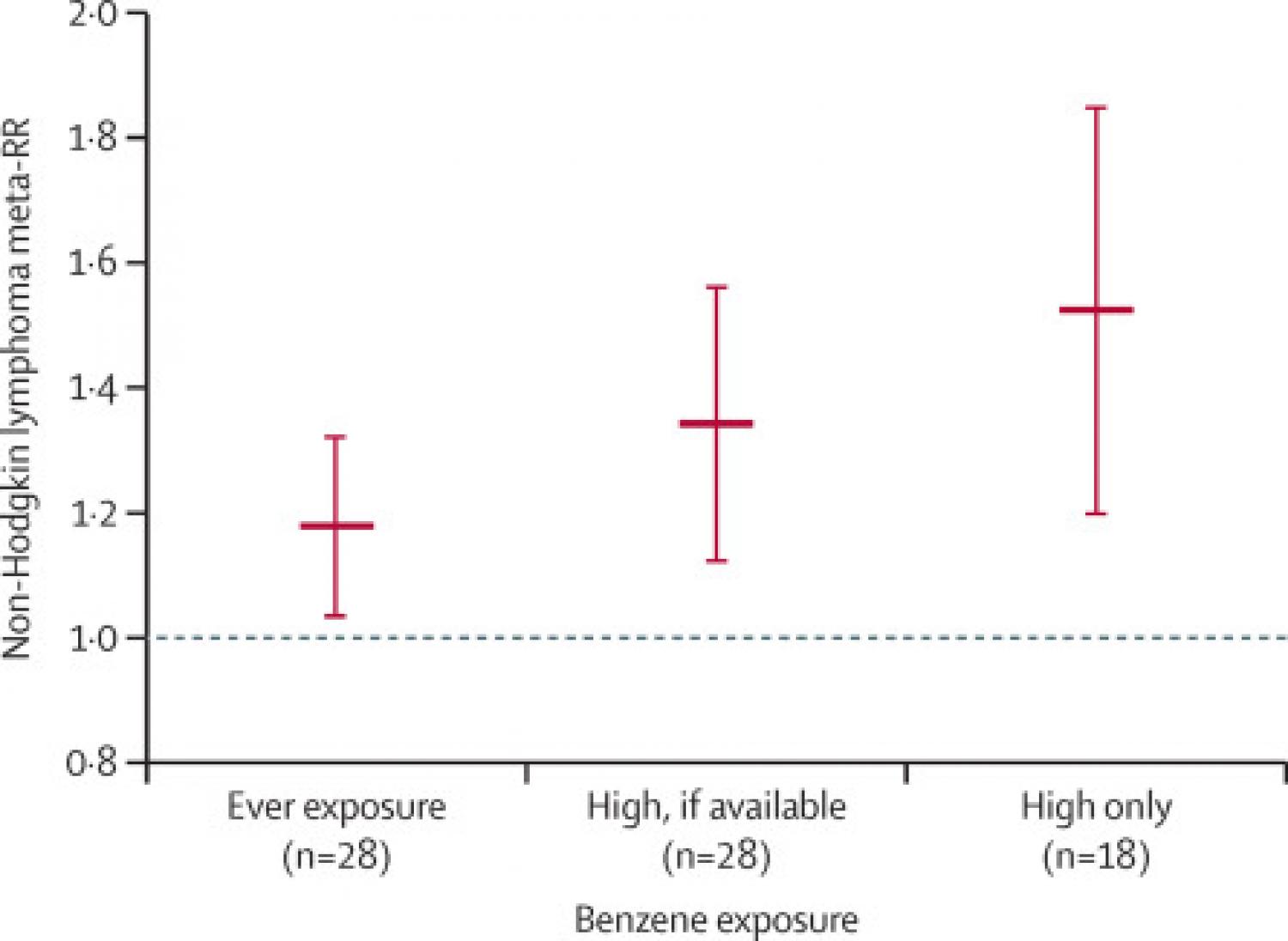
Background: Non-Hodgkin lymphoma comprises a heterogeneous group of cancers with unresolved aetiology, although risk factors include environmental exposures to toxic chemicals. Although the ubiquitous pollutant benzene is an established leukemogen, its potential to cause non-Hodgkin lymphoma has been widely debated. We aimed to examine the potential link between benzene exposure and risk of non-Hodgkin lymphoma in humans by evaluating a wide array of cohort and case-control studies using electronic systematic review. Methods: We did a comprehensive systematic review and meta-analysis of all qualified human epidemiological studies that assessed the relationship between benzene exposure and non-Hodgkin lymphoma. We queried the PubMed and Embase databases for relevant articles published before June 5, 2019, and applied the SysRev platform for study selection. All peer-reviewed human cohort and case-control studies that reported non-Hodgkin lymphoma risk estimates specifically for benzene exposure were eligible for inclusion. Studies that calculated relative risks (RRs) for industries or job types without identifying those specifically exposed to benzene, that combined non-Hodgkin lymphoma with other cancer types, or that reported many different solvent exposures together were excluded. From each study, two investigators independently extracted information on the study design, location, years, sample size, participation rates, age, sex, sources of cases and controls, diagnosis, histological verification, exposure assessment, results, adjustment, and statistical analysis, and subsequently assessed study quality. We calculated the meta-analysis relative risk (meta-RR) and CIs using the fixed effect and random effect models, as well as assessing publication bias. Findings: Our search yielded 2481 articles. After screening and removal of duplicates, 20 case-control studies and eight cohort studies were included in our meta-analysis, which included a total of 9587 patients with non-Hodgkin lymphoma. We reported an increased meta-relative risk (meta-RR) of 33% in highly exposed groups, when data were available (meta-RR 1·33 [95% CI 1·13–1·57], n=28). The meta-RR rose to 1·51 (1·22–1·87, n=18) in the studies that provided results specifically for highly exposed individuals. In particular, we reported a doubling of this risk for diffuse large B-cell lymphoma, a major non-Hodgkin lymphoma subtype (1·67 [1·01–2·77]). We also detected increased risks for follicular lymphoma (1·47 [0·95–2·27]) and hairy cell leukaemia (1·77 [0·99–3·16]), though they were not statistically significant. Funnel plot, Egger's test (p=0·77) and Begg's test (p=0·98) did not show evidence of publication bias. We evaluated the major aspects of causal inference and found evidence to support all the Hill considerations for assigning causation. Interpretation: Our findings suggest a causal link between benzene exposure and non-Hodgkin lymphoma, especially for diffuse large B-cell lymphoma. Funding: National Institute of Environmental Health Sciences.
