Elsevier, American Journal of Kidney Diseases, Volume 79, February 2022
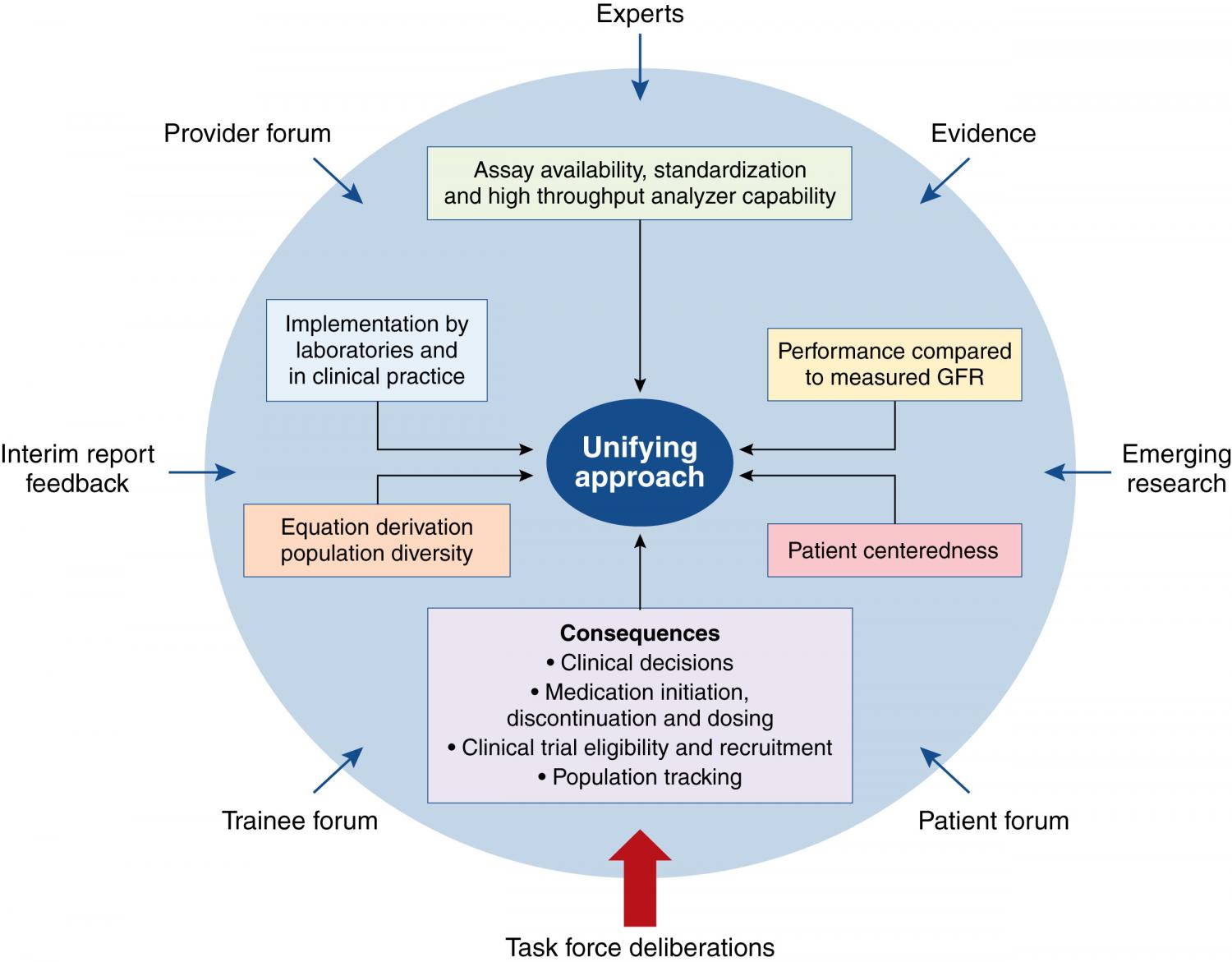
Background: In response to a national call for re-evaluation of the use of race in clinical algorithms, the National Kidney Foundation (NKF) and the American Society of Nephrology (ASN) established a Task Force to reassess inclusion of race in the estimation of glomerular filtration rate (GFR) in the United States and its implications for diagnosis and management of patients with, or at risk for, kidney diseases. Process & Deliberations: The Task Force organized its activities over 10 months in phases to (1) clarify the problem and evidence regarding GFR estimating equations in the United States (described previously in an interim report), and, in this final report, (2) evaluate approaches to address use of race in GFR estimation, and (3) provide recommendations. We identified 26 approaches for the estimation of GFR that did or did not consider race and narrowed our focus, by consensus, to 5 of those approaches. We holistically evaluated each approach considering 6 attributes: assay availability and standardization; implementation; population diversity in equation development; performance compared with measured GFR; consequences to clinical care, population tracking, and research; and patient centeredness. To arrive at a unifying approach to estimate GFR, we integrated information and evidence from many sources in assessing strengths and weaknesses in attributes for each approach, recognizing the number of Black and non-Black adults affected. Recommendations: (1) For US adults (>85% of whom have normal kidney function), we recommend immediate implementation of the CKD-EPI creatinine equation refit without the race variable in all laboratories in the United States because it does not include race in the calculation and reporting, included diversity in its development, is immediately available to all laboratories in the United States, and has acceptable performance characteristics and potential consequences that do not disproportionately affect any one group of individuals. (2) We recommend national efforts to facilitate increased, routine, and timely use of cystatin C, especially to confirm estimated GFR in adults who are at risk for or have chronic kidney disease, because combining filtration markers (creatinine and cystatin C) is more accurate and would support better clinical decisions than either marker alone. If ongoing evidence supports acceptable performance, the CKD-EPI eGFR–cystatin C (eGFRcys) and eGFR creatinine–cystatin C (eGFRcr-cys_R) refit without the race variables should be adopted to provide another first-line test, in addition to confirmatory testing. (3) Research on GFR estimation with new endogenous filtration markers and on interventions to eliminate race and ethnic disparities should be encouraged and funded. An investment in science is needed for newer approaches that generate accurate, unbiased, and precise GFR measurement and estimation without the inclusion of race, and that promote health equity and do not generate disparate care. Implementation: This unified approach, without specification of race, should be adopted across the United States. High-priority and multistakeholder efforts should implement this solution.

